How Doctors Minimize the Risk
Doctors follow several precautions to ensure the risk of a biopsy is next to zero. Image credit: ShutterstockMedical professionals do not ignore the possibility of seeding; they have developed specialized techniques to prevent it. If you are undergoing a your medical team is likely using one or more of the following safeguards:
- Coaxial needles: Many doctors use a “sleeve” or “sheath” technique. A larger hollow needle is inserted up to the edge of the tumor, and then a smaller biopsy needle is passed through that sleeve to take the sample. When the biopsy needle is pulled back, it stays inside the sleeve, ensuring the tissue sample never touches the healthy tissue along the path.
- Surgical planning: When a surgeon performs a biopsy on a tumor they intend to remove later, they carefully plan the path of the needle. They often ensure the biopsy track is located in a section of tissue that will be entirely removed during the subsequent surgery. This way, even if seeding occurred, the entire area is cut out.
- Fine-Needle precision: The use of smaller needles reduces the displacement of tissue, further lowering the already slim chances of cell migration.
The Greater Danger: The “Wait and See” Approach
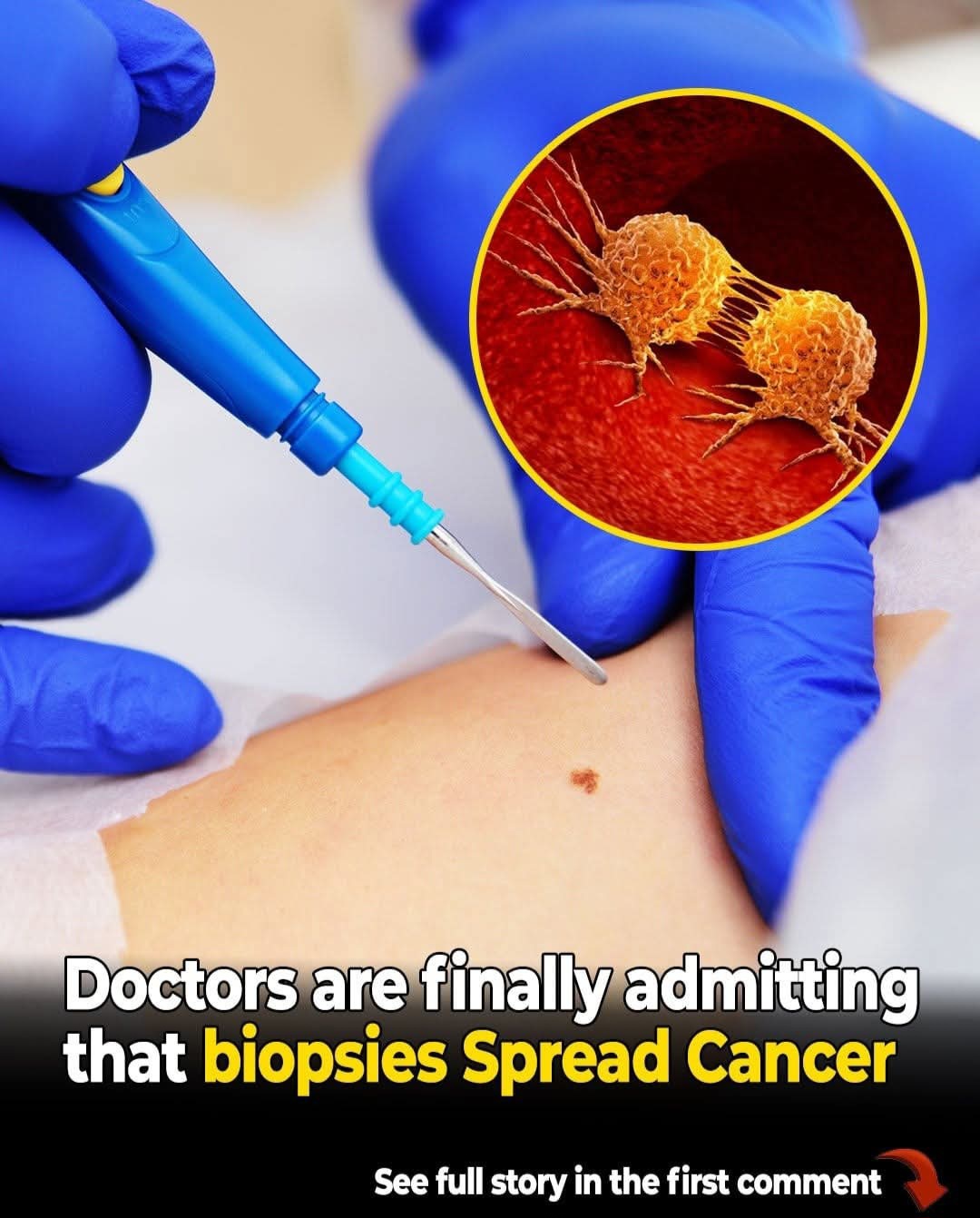
The fear of a biopsy spreading cancer can lead to a much more dangerous outcome: avoiding the biopsy altogether. Cancer is most treatable, and often curable, when caught early. Delaying a diagnosis allows the tumor to grow naturally. Unlike the theoretical risk of a needle spreading cells, the risk of an untreated tumor spreading on its own through the lymphatic system or the bloodstream is a virtual certainty if left long enough.
Without a biopsy, doctors are “flying blind.” They cannot know if a tumor requires aggressive chemotherapy or a simple localized surgery. Using the wrong treatment because of an incomplete diagnosis can be fatal. In the world of oncology, information is the most powerful weapon a patient has. The biopsy provides that information.
Addressing the “Admissions”
The headline suggests that doctors are “finally admitting” this risk, implying a shift in medical honesty. In reality, the medical community’s openness about the risks of any procedure, whether it’s a biopsy, a routine surgery, or a new medication, is part of the standard of informed consent.
Doctors discuss these risks because they want patients to be partners in their care. The American Society of Clinical Oncology (ASCO) and other leading bodies provide detailed information on these topics not to scare patients, but to dispel the myths that flourish in the absence of clear communication. By acknowledging that a risk, however tiny, exists, doctors can explain why they take specific precautions to manage it.